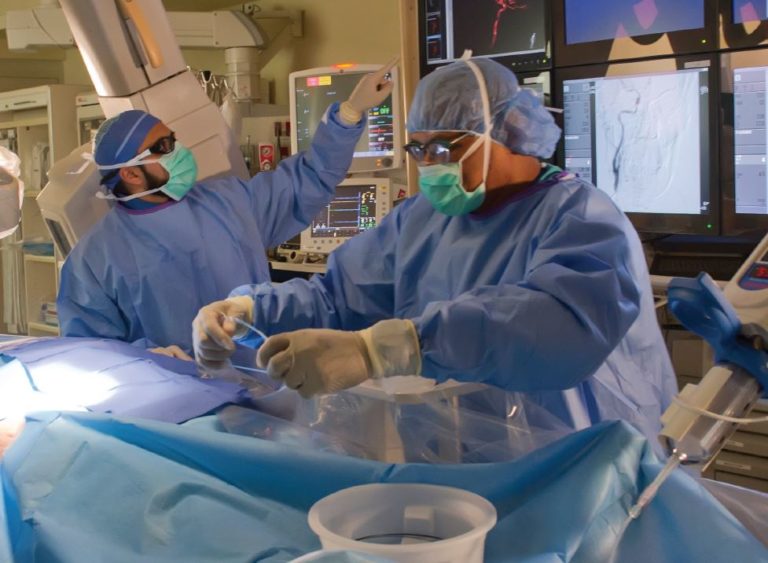
Hamza A. Shaikh, MD, Co-Director, Neurointerventional Surgery, performs a thrombectomy on a stroke patient in the Cooper Catheterization Laboratory.
Cooper is the first hospital in South Jersey to earn Comprehensive Stroke Center certification from the Joint Commission and the American Heart Association/American Stoke Association. This makes Cooper part of an elite group of hospitals. It’s a big deal.

Tudor G. Jovin, MD
“This national certification means that we have undergone rigorous scrutiny and met the highest standards for the full spectrum of stroke care, from the speed with which patients receive reperfusion therapies to the appropriateness of post-discharge care,” explains Chief of Neurology and Chairman of Cooper’s Neurological Institute, Tudor G. Jovin, MD.
“It’s very different from the state definition of comprehensive stroke care, which requires a much less sophisticated system and infrastructure,” he adds, “which explains why there are so many more state-designated stroke centers than Joint Commission-certified ones.”
One significant difference is the depth and breadth of stroke-related specialty and subspecialty expertise that is available at Cooper 24/7.
“There may be other comprehensive stroke centers in the region, but they do not have the number of board-certified and –eligible vascular neurologists that we have,” Dr. Jovin says. “We also have neuro-interventionalists, vascular neurosurgeons, neuroradiologists, and neuro-intensive care experts on site at all times. As a result, I can say with confidence that we are doing interventional procedures with greater efficiency and speed.”
Speed is a critical factor in ensuring a successful outcome when ischemic stroke occurs.
“Restoring blood flow to the brain is exquisitely time sensitive,” Dr. Jovin says, “and we have a very efficient system of throughput that other facilities performing thrombectomies can’t come close to.”
In fact, since Dr. Jovin took the helm of Cooper’s Neurological Institute earlier this year, the stroke team has been consistently achieving door-to-puncture (DTP) times of 20 minutes in the vast majority of cases. DTP is the time it takes from arrival at the endovascular center to the start of the thrombectomy procedure in the neuroangiography suite. It includes the time it takes to perform a neurological evaluation, complete the imaging studies, treat the patient with intravenous tPA if applicable, transport the patient to the neuroangiography suite, and prepare the patient for the intervention. To put that number in perspective, current Get With The Guidelines®- Stroke, the American Heart Association’s performance improvement program, calls for a DTP time of 90 minutes.
“No other comprehensive stroke center or thrombectomy-capable center in this region comes close to what we are doing in terms of door-to-puncture times,” Dr. Jovin emphasizes. “And what we are doing translates into better outcomes.”
Dr. Jovin is one of the nation’s first interventional neurologists and a world-renowned expert in both interventional and non-interventional treatment of stroke and cerebrovascular disorders. He is internationally recognized for his research activities, having recently served as principal investigator for two landmark studies (REVASCAT and DAWN) published in the New England Journal of Medicine in 2015 and 2017, respectively. These studies not only dramatically affirmed the clinical efficacy of mechanical thrombectomy but also were instrumental in expanding the time window for this endovascular treatment of acute stroke beyond the traditional 8-hour time window.
“We demonstrated that in selected patients with large vessel occlusion, the benefit from treatment with mechanical thrombectomy can be seen up to 24 hours,” Dr. Jovin notes. “But that doesn’t mean we can be complacent and take our time,” he stresses.
“In fact, we don’t even base patient selection [for thrombectomy] on time anymore,” he continues. “Each patient has an individual window based on their physiological characteristics. And—most important—regardless of how long it has been since the onset of a patient’s stroke symptoms—earlier treatment leads to better outcomes.”
He goes on to explain that the efficacy of thrombectomy can be measured by the metric of NNTT—the number of patients needed to treat to reduce the disability level from an ischemic stroke from high to low.
“If we take all patients with large vessel occlusion, whether they are in an early or late time window, the number needed to treat is three,” Dr. Jovin says. “To put that in context, giving IV tPA has an NNTT of 9, while angioplasty and stenting for a STEMI is 29.
“So mechanical thrombectomy for stroke is ten times more potent than percutaneous coronary intervention for STEMI,” he adds. “There are few treatments in medicine that have such a strong therapeutic effect.”
It all underscores why seeking care for stroke at a Joint Commission-certified Comprehensive Stroke Center such as Cooper’s is the right choice.
“Just as trauma centers are ranked by the complexity of patients they can handle, I believe stroke centers should be also,” Dr. Jovin says, “so patients with severe stroke and at risk of high deficit are directly transported to a comprehensive stroke center so they receive thrombectomy in the timeliest manner possible.”
Similarly, patients with hemorrhagic stroke have timely access to neurosurgeons with specialized vascular expertise.
“Here at Cooper, we have the entire gamut of stroke care resources available under a single, integrated umbrella,” he adds. “We can offer patients what is truly the highest level of stroke care.”
“No other comprehensive stroke center or thrombectomy capable center in this region comes close to what we are doing in terms of door-to-puncture times. And what we are doing translates into better outcomes.” – Tudor G. Jovin, MD
For more information on Cooper’s Comprehensive Stroke Center, or to refer a patient, please call Dr. Tudor Jovin at 412.726.9974.
